Overcoming Resistance
Overcoming Resistance
To truly protect yourself, you have to let down your guard and look at things you’d rather not face.
Most practitioners facing regulatory discipline are like Tweedle Dee and Tweedle Dum in Alice in Wonderland. They arrive at PBI Education courses ready to do battle, clothed in emotional armor of every kind — denial, repression, defensiveness, rationalization, justification, intellectualization, other-blaming, wishful thinking — all to avoid looking inward.
As the course proceeds, they gradually let go of these defenses and begin to explore the personal vulnerabilities that got them into trouble. It often takes time, however those who complete the process end up far better protected than they started out and no longer weighed down and worn out by their own efforts at resistance.

What do we mean by “resistance”?
We use the term “resistance” to describe a healthcare professional’s inability to fully acknowledge their professional role. Sometimes this means they ignore the legal or regulatory context of their professional work, or they have deficits in their ability to self-reflect. Resistance is manifested by the kinds of emotional armor listed above.
Re-education is the first step
Many participants come to a remedial course outraged at how they are being treated. Rather than accept responsibility for their violation, they blame anyone but themselves. In the U.S., board members are frequently blamed by disciplined practitioners for abusing their authority. Similarly, in Canada practitioners blame members of their regulatory body’s discipline committee. In either case, such “board-bashing” is the first line of resistance many participants have to shed.
“It’s really an educational process at first,” says PBI Education Medical Director, Catherine Caldicott, MD, FACP. Few practitioners are taught anything in professional school about the laws governing their practice. Many are shocked to discover that their license is not a right they have earned but a privilege they must continually prove themselves worthy of.
“Years of frustration have left them feeling helpless and exhausted,” says Caldicott. “It seems to them that patients have all the power, and they have none.” Reorienting themselves isn’t easy. It takes time for practitioners to wrap their heads around the fact that they wield enormous power over the people under their care. Once clinicians grasp the reality of this power differential and the vulnerability of their patients, they begin to understand why both the law and society at large hold them to exceptionally high standards and why regulators insist they take responsibility for measuring up.
Participants also have to realize that their regulator is not in their corner. “Part of people’s initial outrage,” says Caldicott, “comes from thinking their regulatory body is supposed to be looking out for them, when in fact its primary purpose is to protect the public from unprofessional practitioners.”
As each of these realizations settles into place, participants’ outrage begins to fade. Eventually, they come to see the regulator’s disciplinary action not as a punishment for past behavior but as an opportunity to change course and reclaim their career.
Gentle prompts help chip away at resistance
Once course participants begin to accept responsibility for the impact of their actions and choices, it’s time to begin unpeeling the remaining layers of resistance. Once again, education plays a part. The PBI Formula© helps participants understand the various factors, including resistance, that influence how likely they are to commit a violation.

Resistance is represented in the formula as an exponent to illustrate how powerfully it can elevate someone’s potential for committing a professional violation. “You can’t address problems you are unwilling or unable to look at,” says PBI Education founder, Stephen Schenthal, MD, MSW.
Most people aren’t even aware of their resistance and how it is putting their career at risk. “It’s like the magic cloak in Harry Potter that makes things invisible,” says Schenthal. “You can’t see something right in front of you until someone who’s aware of your resistance shows you what’s going on.” Even then, some people refuse to accept that they are being resistant, which means the invisibility cloak remains in place and they continue missing the problem staring them in the face. At that point, violation potential soars to a whole new level.
Course participants help each other overcome resistance
The power of resistance becomes increasingly evident in a course as the instructor moves the discussion past external risk factors, which tend to be less threatening, and starts urging participants to consider their own internal vulnerabilities. At that point, as their anxiety levels start to climb, people begin strapping on their emotional armor. In response, instructors go to work helping participants lower their defenses so they can continue exploring issues they find threatening.
Calling on years of experience and training, instructors know that other people in the course play an important role in this process. “Peers are often less threatening than an authority figure, like an instructor,” says Schenthal. “People are more open to observations and feedback from others they identify with, people who are going through the same thing they are.”
In one course, a nurse insisted that the hug they gave to an upset patient was meant to be comforting, not threatening. After a little probing by the instructor, the nurse admitted also hugging patients who weren’t upset at all. A carefully guided discussion prompted more back-and-forth among participants. As others in the course asked questions and offered suggestions, the nurse gradually came to see how the hug they gave was more about their own need for comfort than it was about the patient’s.
Those providing feedback also benefit. It’s a lot easier to see how defensive others are being than it is to accept your own resistance. And once you spot resistance in someone else, you may begin to see it in yourself as well.
Real progress takes time
Not always, but often, there comes a point when someone eventually needs a stronger push. Knowing when that moment has arrived is tricky. Push too soon and you just make things worse. Wait too long and you risk losing an opportunity.
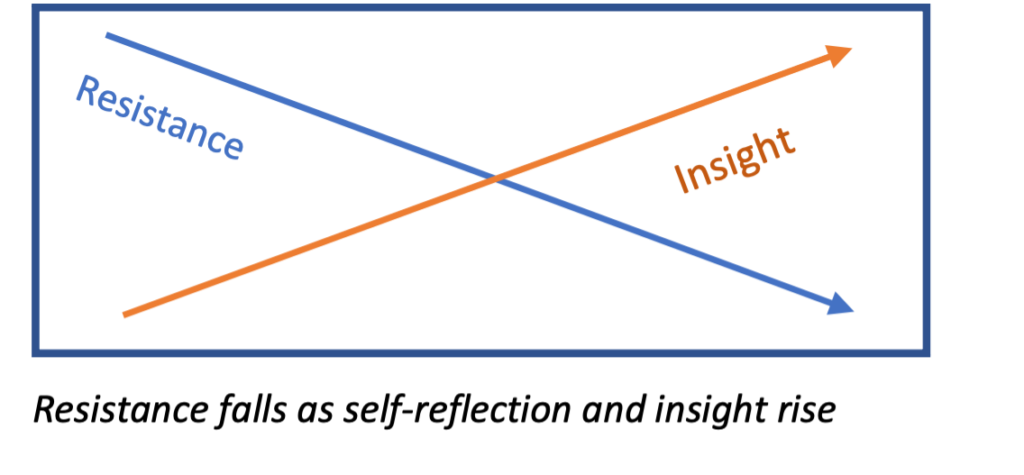
Whether it’s the instructor or other participants who eventually confront someone, confrontations almost always come near the end of a course. “In part, that’s because resistance gradually falls as self-reflection and insight rise, and people simply need enough time for the lines to cross,” says Schenthal.
Once the lines do cross, the process often begins to accelerate, leaving participants eager to keep going even after the course ends. They may feel the need to continue exploring their vulnerabilities or they may be looking for more support as they begin grappling with issues they’ve been resisting for years.
In such cases, many participants enroll in PBI Education’s weekly Maintaining Accountability with Support (MAS-12). These group conversations run for 12 weeks, giving participants a chance to build on what they’ve learned. During this extended course, people also grow to understand and trust each other in ways that foster still more progress.
Clearing a threshold
As gradual as the process is, there does seem to be a point at which it is easier to keep going forward than it is to fall back. Once someone has learned enough about themselves and become sufficiently aware of their own resistance, they cross what Schenthal calls a “threshold.” At that point, he explains, “people are generally a lot happier, a lot more at peace than they have been in a long time. And they don’t want to lose what they have gained.”
To protect themselves from relapsing, PBI Education graduates create a Personalized Protection Plan that addresses their vulnerabilities and risk factors. The plan also includes ways to increase accountability, the one factor in the PBI Formula that can offset the effects of risk factors, vulnerabilities, and even resistance. A good example of an accountability measure is the involvement with an outside observer of some kind — often a supervisor, a colleague, or a mentor — and that person can help a practitioner realize when they are being resistant.
“But it has to be someone who will be straight with you,” says Caldicott. “You want someone who won’t just tell you what you want to hear. But you also need someone you trust, someone who can help you look at things you’d rather not face.”
More to come: Once someone is sensitized to resistance, they are much more likely to realize early on that they’re heading for a fall. The key is paying attention to warning signs. More on this topic in an upcoming blog, be sure you are subscribed to be the first to know when a new blog is published.
Would you like to learn more about the PBI Formula© and assess your own resistance level, risk factors, and vulnerabilities? Click here to enroll in the self-paced 2 CME online course, Navigating Professional Boundaries in Health Care.
Takeaways
- Resistance includes denial, repression, defensiveness, rationalization, justification, intellectualization, other-blaming, and wishful thinking.
- Your professional license is a privilege you must continually prove worthy of.
- Disciplinary action gives you an opportunity to change course and reclaim your career.
- Because it powerfully prevents you from accepting responsibility and making changes, resistance is depicted as raising your violation potential exponentially.
- It takes time, sometimes more than a single course, to gain the insights and trust you need to overcome resistance.
- Accountability diminishes violation potential in part by enhancing awareness of resistance.
